Following on from my previous blog about golf injuries, I thought I would look at another common complaint. Lateral hip pain is certainly one of the most common problems we see walk through the door and it is also one of the most frustrating to treat and manage.
What is Lateral Hip Pain?
Firstly, there are many different structures that could be causing pain through your hip such as osteoarthritic changes, your Sacral Iliac Joint (SIJ) or your lower back so it is important that you have a full assessment in order get the right diagnosis from the start.
The condition I am going to discuss is trochanteric pain syndrome and the role the gluteal tendons play in it. This syndrome can cause pain on the outside of the hip, which can spread down to the knee and run into the buttock.
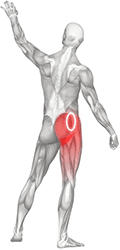
Generally these symptoms are aggravated with prolonged walking, going up and down stairs and lying on the involved side. Initially these symptoms where often thought to be associated with inflammation to the bursa on the side of the hip. This was known as trochanteric bursitis. However with improvements in investigations such as MRI and Ultrasound clinicians now believe that the tendons of the gluteus medius and the gluteus minimus muscles are more involved. We believe that the pain that is experienced is a result of these tendons being over loaded and losing their structural integrity resulting in them breaking down. This condition is known as a tendinopathy.
How does this happen?
This overloading of the tendons on the outside of your hip is often the result of poor control and balance through the pelvic and lower back regions. On assessment there is often a weakness through the muscle groups that are associated with stabilizing the hip joint. A simple way of assessing this is to look at how well the patient is able to balance on 1 leg. The picture below shows how an unstable pelvis will tilt on a single leg stand and put pressure on the gluteus medius muscle.
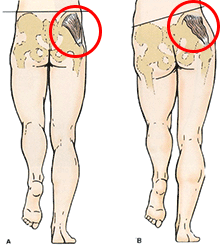
Gluteus Medius
When looking into the history of our patients with this injury there is generally an episode of increased loading or an increase in activity, such as a day in the garden or starting a new exercise group. This spike in activity can aggravate the tendons of the gluteus medius and minimus muscles if there is not suitable stability through the pelvis. Once these tendons have been aggravated they are then easily re-aggravated during daily activities such as going up and down stairs or from sleeping on the affected side.
Recommended Therapies : Dry Needling
A major part of physiotherapy intervention for trochanteric pain is based on correcting this imbalance, which can be done through specific strengthening and conditioning programs. However, before any of these exercises can be implemented it is important for the pain levels to be well controlled and this is where dry needling comes in. There are many treatments that are used to control pain levels and sometimes it is necessary for medical intervention, but I find Dry Needling is an effective option.
What is Dry Needling?
Dry needling is where acupuncture needles are used in specific regions of different muscle groups to inhibit and suppress how the body processes pain. Unfortunately the longer the pain has been present the longer it takes to control and therefore time frames can vary. Once the pain levels are controlled then we can introduce specific loading exercises for the tendon and ultimately a full strengthening program to restore pelvic stability.
As I mentioned at the beginning, this can be a very frustrating condition to treat and to get on top of. In chronic conditions where pain has been present for a number of months it is often necessary for onwards referrals to medical practitioners to get to a position where a conditioning program can be tolerated. Therefore it is important to get an early assessment and diagnosis.
