Physio Blogfrom the team at South Coast Physiotherapy
Displaying items by tag: knees
Happy Knees
The importance of addressing Knee Health in treating knee OA
Osteoarthritis (OA) is a degenerative process involving the break down of cartilage at a joint leading to pain, swelling and loss of function. The prevalence of knee OA has doubled in the last 50 years and is a major burden on health care services around the world. As a result researchers and health organisations are constantly looking at the best ways to manage this condition. Clinical practice currently suggests that treatments should be directed away from structural/mechanical models which are based on restoring the knee structure and instead should be directed more towards addressing the health of the knee. Understanding that OA is more than just tissue breakdown and that if treatments can control the inflammatory process and tissue sensitivity associated with OA, that there will be an improvement in knee function, pain levels and patient quality of life.
Cartilage is not related to pain
Historically treatments have been structurally and mechanically based, directed towards restoring the lost cartilage either through different types of injections or supplements. However we know that the breakdown of cartilage is not correlated to knee pain and therefore focusing treatment on restoring cartilage will not necessarily make the knee feel or function any better.
So why doesn’t my exercise routine work?
Since I qualified as a physiotherapist back in the early 2000s exercise has been one of the first line treatments for the condition with focus on restoring range of motion and improving muscle strength. Studies have shown that it can effectively reduce pain and improve function and when you add this to the extensive list of health benefits that are associated with exercise it is not surprising that it is the first port of call. However even with exercise we need to ensure that it is being directed at improving knee health rather than purely strengthening the knee or replenishing articular structures. Exercise alone is not a sufficient intervention. It needs to be incorporated into addressing knee health and failure to do this is a major reason why prescribed exercise routines sometimes do not work.
How do we incorporate an exercise program into a knee health model?
The exercise program itself is not the initial priority. When treating a symptomatic OA knee the clinician is not trying to purely restore muscle strength but instead is addressing a complex inflammatory process being driven and influenced by many factors and comorbidities. Addressing these is the first step and once the patient has a good understanding of this and the clinician has an understanding of the goals and beliefs of the patient then a suitable exercise program can be prescribed. As a result the exercises are specific to each patient rather than a generic ‘recipe book’ style program. They can be pilates based, gym based, yoga based, home based, water based or any combination of different exercises, what ever works for the patient and is suitable for their knee and their general health at that point. It is therefore beneficial that when starting a program aimed at helping an OA knee that the individual seeks guidance from a trained health practitioner, such as a Physiotherapist, to ensure that the program fits a ‘knee health model’ rather than purely focusing on structural deficits. Unfortunately in some cases knee replacement surgeries are still required but even post surgery following this model will ensure the best rehabilitation.
Is Running Safe for my Knees?
For a long time running has been associated with increased risks of degenerative hip and knee injuries, in particular Osteoarthritis (OA). This association has been so ingrained into public and professional perception that health practitioners have gone as far as advising people to avoid running in a bid to reduce the risks of OA changes.
However these beliefs have been recently questioned when researchers compared a sedentary group of non runners with a group of recreational runners and found that the non runners suffered significantly more OA changes than the running group.
It is important to note that these studies were carried out on healthy subjects with no pre existing knee injuries and also that when they looked into elite runners they found increased risks of OA changes.
As health professionals these findings allow us to reassure patients that they can take advantage of the multiple health benefits of running and have less risk of OA than if they were sitting on the couch.
Even if there are preexisting injuries to the knees we can get people back running with a suitable rehabilitation regime and a gradual return to running program.
With our new running software at South Coast Physiotherapy we are now in the perfect position to offer assessments and programs to get people back running. Give the clinic a call and take advantage of all the benefits that getting back to running can offer.
Skiing injury Prevention
With both Australia and New Zealand having good snow seasons this year and following a recent run of patients suffering snow related injuries I have decided to write this blog on injury prevention when on the slopes.
Risk of Injury
Although skiing and snow boarding are generally associated, as high injury risk activities recent research looking at the prevalence of these injuries has shown a recent decline. The numbers have reduced from 5 – 8 injuries per 1000 skiers to 2 – 3 per 1000.

Research has also shown that the most common injuries in skiing are to the knees which accounts for ⅓ of all injuries and that in snowboarder’s injuries to the wrists are the most common. A study in Japan showed that snowboarders had twice the injury rate of skiers and interestingly a study looking at a terrain park in Canada showed that snowboarders who were listening to music were less likely to have an any injury but more likely to have an injury which resulted in them being taken to the emergency department!
When looking at preventing injuries there are obviously areas that we have no control over, which can increase the chances of injury. These can include poor visibility, the quality of the snow and crowded pistes. However there are also many areas that we can control such as wearing protective garments including wrist protectors and helmets.
Conditioning
One area that has been proven to reduce injuries in skiing is through skiing specific physical conditioning. With snow based disciplines, as with the majority of sports, it is important to be balanced and maintain good alignment and weight distribution through your trunk and lower limbs. However, unlike a lot of other sports, with skiing you are trying to maintain a relatively static position while travelling fast down a hill. This, therefore, is going to require different muscle activity and joint positioning compared to an activity such as running, meaning a specific conditioning program is necessary.
Alignment
When looking at skiing you need to assess your alignment to avoid excessive loading through your knees and hips. A lot of pain experienced through the front of the knee with skiing is a result of over loading through the patella femoral joint (where the knee cap sits). When you go into your skiing position your knees should be in line with your 2nd to 3rd toes and not dropping in towards the inside of your big toes. (as shown in the figure below)
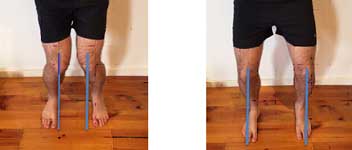
Knee dropping inside the big toe: incorrect Knee in line with the 2nd to 3rd toes: correct
Once you have addressed this imbalance it is then important that you are achieving the correct hip and knee movement. As you go into the skiing position your weight needs to be more into the front of your feet rather than at the back as this will distribute your weight in a more uniform pattern through your skis giving you greater control. This is slightly different to the sit stand motion we use on a daily basis where our weight is distributed more through our heels and therefore it can take a little bit of training to get right.
Strength
In order to maintain this alignment it is vital to have good strength through the gluteal and quadriceps muscle groups. Due to the down hill nature of skiing the quadriceps need to be worked eccentrically. This means they are worked from a straight knee position to a bent knee position and the quadriceps muscles are lengthening. Two of the best exercises to achieve this are deep squats and vertical split squats (as shown below).

Vertical Split squats
Proprioception & Endurance
Proprioception is the body’s awareness of where it is in space and is therefore a very important factor in reducing injury risk, especially when skiing in poor visibility. Simple ways to address this are through balance exercises such as single leg standing with eyes closed.
Similar to other sporting injuries, skiers and snow borders are more vulnerable as they get more fatigued and this can be addressed through generic cardiovascular exercises such as cycling and running.
It is important to mention that these guidelines are for uninjured skiers. If you have an ongoing complaint or old injury then a more specific personal program would be necessary.
Happy Skiing……